The trust–success ratio: Why building trust is the cornerstone of PPIE (Public Patient Participation Inclusive and Engagement) – A patient’s perspective
Written by Dr Sondra Butterworth, CEO RareQoL, community psychologist and patient advocate
Estimated reading time: 7 minutes


As someone living with long-term health conditions and from a rare disease family, I have spent much of my life navigating the NHS and healthcare systems. My experiences as a patient, advocate and psychologist have shaped my understanding of what PPIE (Patient Participation Inclusion and Engagement) and genuine, inclusive research should look like. Trust is the invisible thread that binds patients, researchers and organisations together. For those involved in patient engagement, health equity, patient centricity initiatives and patient recruitment for clinical trials: I believe, must not underestimate the importance of trust and its relationship to the success of your projects and initiatives.
The three levels of trust
When we talk about inclusion in research, especially within PPIE, we must ask: How important is trust at three levels: the person, the system and the organisation? For those of us who have felt the weight of exclusion or misunderstanding, this question is at the heart of meaningful engagement.
- Personal (micro): Trust between the participant and the researcher. This is about researchers understanding our lived experience: ethnicity, gender, culture, health journey. Ensuring informed consent is truly understood and providing clear, respectful communication.
- System/process (meso): Trust in the research process itself: e.g. recruitment process or independent, diverse review boards, robust data security and transparent processes for data collection and analysis.
- Organisational (macro): Trust in the research institution or funder. We look for ethical track records, genuine community engagement and clear policies addressing historical injustices. Remember oral history: patients talk and pass down stories of their experiences.
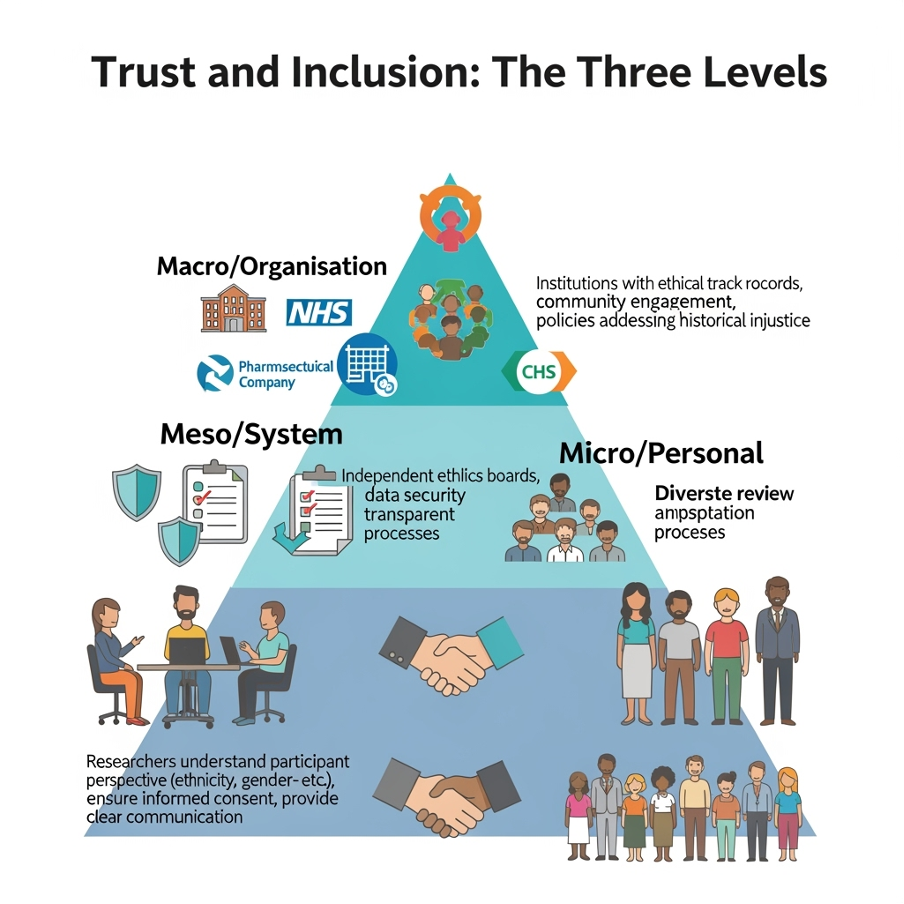
1: Levels of trust
Adapted from Bronfenbrenner’s Ecological Systems Theory Bronfenbrenner, U. (1977).Toward an experimental ecology of human development.American psychologist, 32 (7), 513
The trust–success ratio: Why history and barriers matter
Trust is shaped by lived experience and history. For many rare disease families and people from ethnic minority backgrounds, mistrust of healthcare and research systems is rooted in direct experience and collective memory. The story of Henrietta Lacks1, whose cells were taken without consent, and the Tuskegee Syphilis Study2, where Black men were deceived, are stark reminders of why trust is fragile.
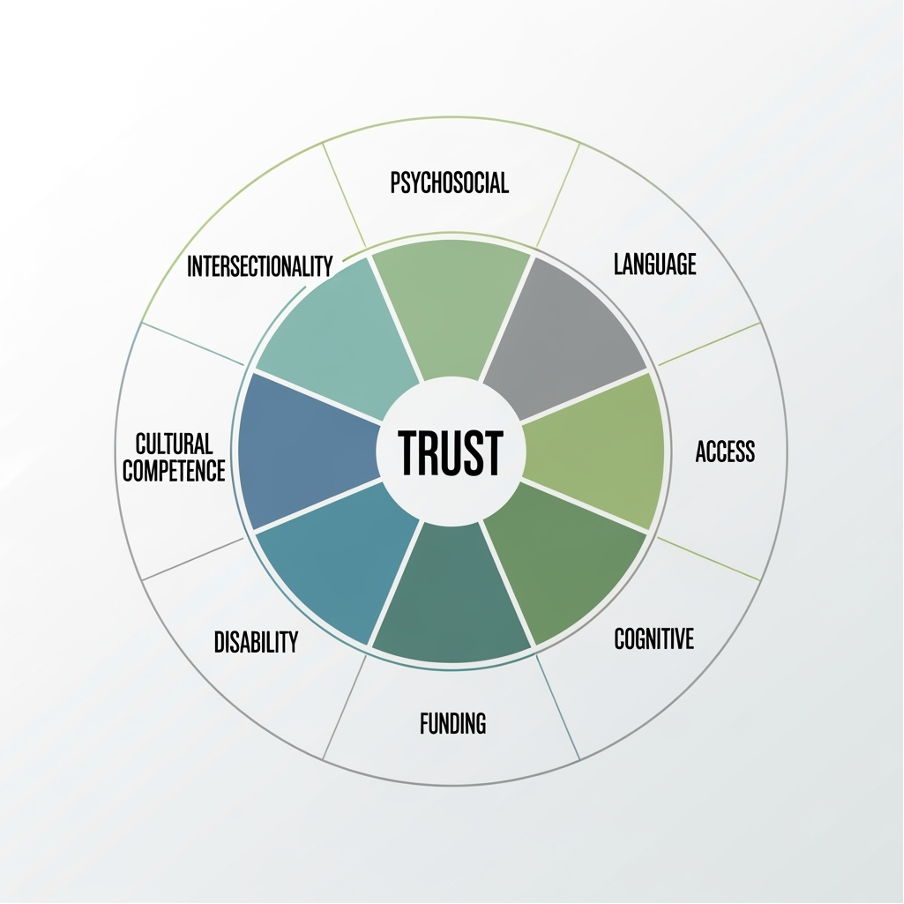
Figure 2: Barriers to inclusion: trust at the core
RareQoL have partnered with associate professor Dr Andrew Mitchell from the University of Chester UK and developed EDIRA (Equality diversity and Inclusive Research Association). In one of our research projects we identified nine barriers to inclusion
At the centre of all these is trust. From this perspective started the assumption that there is a relationship between trust and success which we discussed in our Building Trust Symposium in 2024.
The Trust–Success Ratio: Just consider: could there be a relationship between trust and success? The greater the trust, the greater the success in achieving true inclusion and meaningful outcomes.
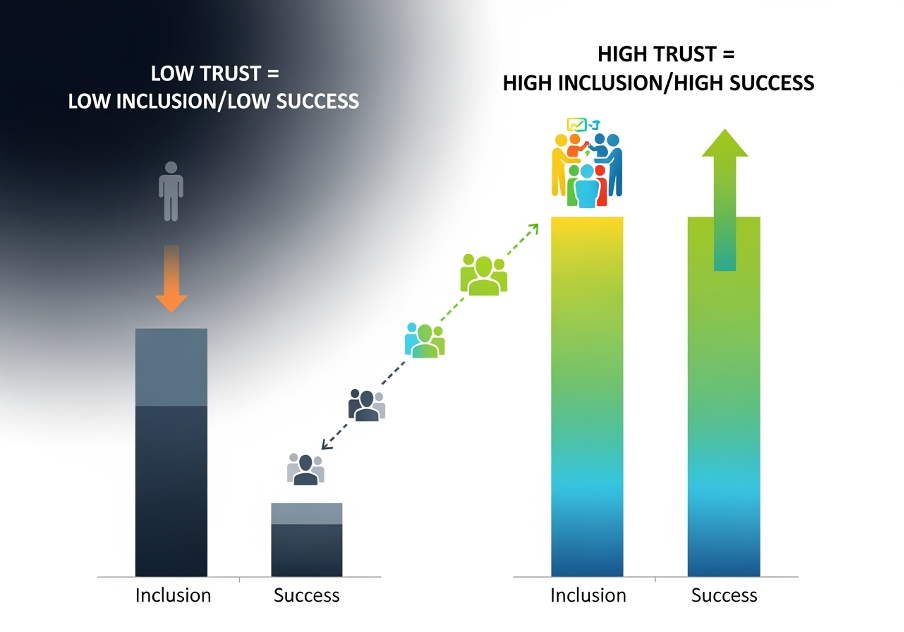
Figure 3: The trust – success ratio™
Practical suggestions: Building trust—a patient’s perspective
From a patient perspective, I know the difference it makes when researchers and healthcare professionals genuinely seek to understand my lived experience. Building trust isn’t about ticking boxes—it’s about listening, co-creating and acting with empathy and transparency. Below, I’ve outlined the nine barriers to inclusion identified through EDIRA’s work, alongside practical suggestions for building trust from my perspective as a patient.
How to build trust: a patient’s perspective
| Barrier to inclusion | How to build trust: A patient’s perspective |
| 1. Psychosocial factors | Acknowledge emotional and mental health impacts. Offer psychosocial support and create safe spaces. Be trauma informed with awareness of impact of diagnostic journey. |
| 2. Access to communities | Partner with local advocates and patient groups. Use trusted messengers and community-led outreach to ensure everyone feels welcome and valued. |
| 3. Language | Provide information in multiple languages (if possible) and plain English. Use interpreters and culturally relevant examples to make research accessible. |
| 4. Cognitive ability | Simplify consent forms and communication. Use visuals, easy-read formats and check for understanding—never assume comprehension. Consider neurodivergent participants. |
| 5. Economic status | Reimburse travel and time, offer virtual participation and remove financial barriers. Be transparent about compensation and costs. Be aware of financial rewards and impact on benefits. |
| 6. Funding | Advocate for dedicated funding to support inclusion and engagement. Make sure resources are available for outreach, translation, accessibility and dissemination of finding. |
| 7. Disability | Risk assess online and virtual spaces. Ensure venues, materials and digital tools are accessible. Ask patients directly about their access needs and act on their feedback. |
| 8. Cultural competence | Invest in cultural awareness and trauma-informed training for all staff. Involve people from diverse backgrounds in co-design and delivery. |
| 9. Intersectionality | Recognise that many patients face multiple, overlapping barriers. Be aware of the impact of intersectionality and health equity. |
Building trust to Improve PPIE: A call to action
Understanding the patient perspective is not optional—it’s essential.
Consider a few key questions.
Question: Can trust be bought?
Answer: No!
Question: Can trust be built?
Answer: Yes!
Question: How long does trust-building take?
Answer: It depends on how much mistrust exists, how deep the mistrust is and how long the feelings of mistrust have lasted
Question: How do we begin to build trust?
Answer: We start by working with trusted advocates and patient groups: especially those who are trauma informed and understand the diagnostic odyssey from a patient and family perspective. Consider The Effect! The messenger matters as much as the message: lived experience and/or empathy breaks down barriers. Who is delivering your recruitment message?
As the NHS launches its10-Year Health Plan3 and develops it’s Patient Charter we have to consider the question: How can we develop a Patient Charter, or any plan for real inclusion, without first building trust?
Trying to build a Patient Charter or improve research recruitment without authentic patient involvement is impossible. We cannot design for patients without patients. We cannot build trust without a shared understanding.
Building trusting relationships is not easy, especially for those of us who have been excluded or misunderstood. Trust cannot be bought it can only be earned, and that takes time, a willingness to learn and listen. The deeper and longer the mistrust, the longer it will take to rebuild.
At EDIRA, we’ve brought together EDIRA partners, Rare Community Network members, collaborators and sponsors to showcase real-life examples of trust-building with impactful outcomes. Through our “Let’s COCO and Celebrate the Doers” event, we spotlight those who don’t just talk about trust but live it. These stories show that trust, once earned, can transform lives and systems.
Connect with Sondra
References
[1] https://bloodcancer.org.uk/news/the-stolen-legacy-of-henrietta-lacks/
[2] https://www.cdc.gov/tuskegee/about/index.html
[3] https://www.gov.uk/government/publications/10-year-health-plan-for-england-fit-for-the-future/fit-for-the-future-10-year-health-plan-for-england-executive-summary
in the loop lets you stay informed with all the latest issues from the world of RARE. To access more in the loop articles click below.


